Bronchiectasis (Bronchiektasien)
General information:
- Low incidence in industrialised nations.
- Permanent localized or diffuse abnormal dilatation (fusiform, cylindrical, saccular) of the segmental and subsegmental bronchi and their branches.
- Principal areas of involvement: Lower lobes most often affected, followed by the right middle lobe and the lingula.
- Etiology: chronic suppurative lung disease, repeated pulmonary infections and poor clearance of lung secretions. That leads to destruction of the bronchial wall tissue with bronchomalacia and muscular hypertrophy. Brochus obstruction may worsened by compression due to enlarged lymph nodes.
- Congential bronchiectasis are rare (Klippel – Feil – short neck, rib anomalies - or the Kartagener syndrome: ciliar dyskinesis, situs inversus, pansinusitis and bronchiectasis, infertility).
- Cystic fibrosis is the most common underlying disease causing bronchiectasis. A foreign body may also cause local bronchiectasis.
Symptoms:
- Fever, cough, significant amounts of purulent sputum.
- Physical activity (change of position) stimulates paroxysmal coughing.
- Musical rales may be detected by auscultation.
- Hemoptysis may occur.
- Clubbing of the fingers in the late stages.
Diagnostic workout:
- High – resolution CT scan instead of bronchography.
- Bronchoscopy and biopsy (ciliar morphology).
- Ventilatory perfusion lung scannings.
- Evaluation for cystic fibrosis.
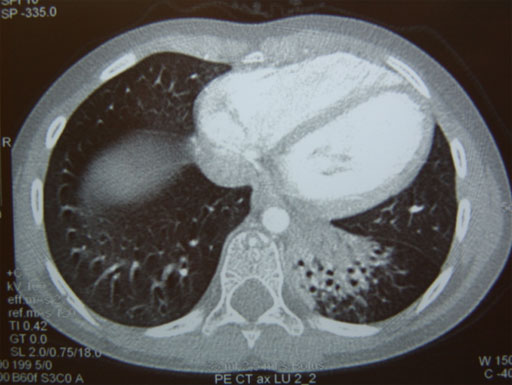
Indication for operation:
- Recurrent lung infections in relation to localized bronchiectasis.
Treatment/Operation:
- In early stages conservative treatment (antibiotics, mucolytica, good pulmonary toilet).
- Lobe or segment resection. The operation may be difficult because of postinfectious pleural adhesions and lymph node hypertrophy.
- In patients with diffuse bronchiectasis lung resecion may be required (Cystic fibrosis of the lungs is the main indication for lung transplantation in childhood).
Postoperative management:
- Chest tubes may be removed if the lung is fully expanded and drainage volumes decrease below 20 to 50cc during a 24 hour period.
Prognosis:
- Good. Relapse may occur in patients with poor clearance of lung secretions (mind the underlying disease, CF, Kartagener – Syndrome).



